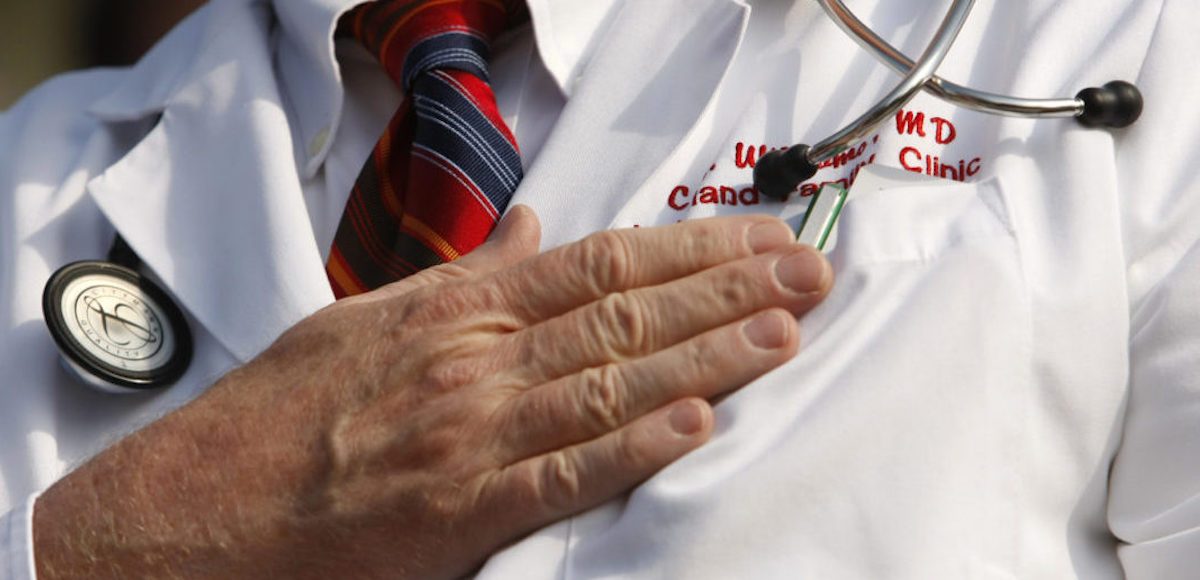
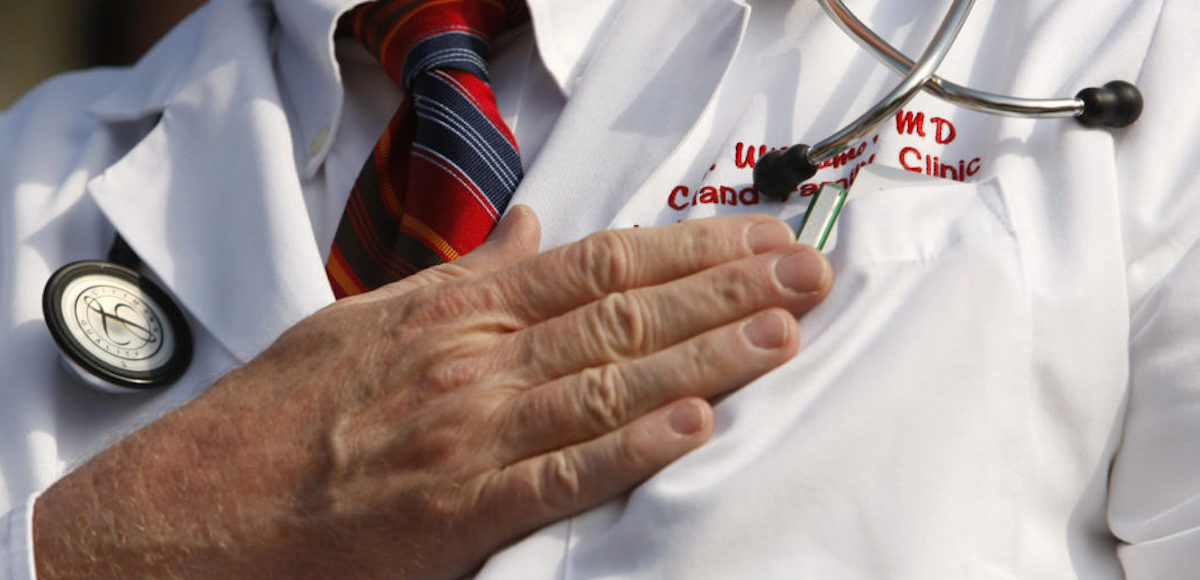
A doctor puts his hand over his chest during a “House call” rally against proposed healthcare reform legislation at the Capitol in Washington November 5, 2009. (Photo: Reuters)
The Centers for Medicare & Medicaid Services (CMS) said average premiums have dropped for the first time since the implementation of the federally-run health exchange in 2014. The average premium for the popular, second-lowest cost silver plans (SLCSP) for the 2019 coverage year will drop by 1.5%, with much larger drops in particular states (see below).
CMS Administrator Seema Verma argued the average premium declines — coupled with increased issuer participation for the year — vindicate the numerous actions taken by the Trump Administration to stabilize what previously were failing health exchanges.
“President Trump’s Administration took action to address the skyrocketing price of health insurance, and now we are starting to see the results,” Administrator Verma said in a statement. “Despite predictions that our actions would increase rates and destabilize the markets, the opposite has happened.”
On Inauguration Day, President Donald Trump signed an executive order placing a freeze on federal regulations and easing burdensome regulations mandated by ObamaCare. Within a month of Inauguration Day and at the president’s direction, CMS put together a market stabilization rule and used its waiver authority to approve reinsurance programs in 7 states, resulting in lower premiums.
President Trump, working closely with Senator Rand Paul, R-Kty., signed an executive order expanding healthcare associations and allowing the purchase of insurance across state lines. Prior to the plan, insurers were dropping out of the exchanges one after another.
For the 2016 plan year, there were 237 medical qualified health plan (QHP) issuers operating on federal exchanges. By 2017, there were only 167 medical QHP issuers, a decline of roughly 30%. By 2018, more than half of U.S. counties on the federal platform had only one issuer. A CMS study found 1,200 counties, or roughly 40% of the country, would have only one issuer in 2018 if the actions weren’t taken.
“The drop in benchmark plan premiums for plan year 2019 and the increased choices for Americans seeking insurance on the exchanges is proof positive that our actions are working,” Administrator Verma added. “While we are encouraged by this progress, we aren’t satisfied. Even with this reduction, average rates are still too high. If we are going to truly offer affordable, high quality healthcare, ultimately the law needs to change.”
While the Democratic supermajority in the 111th U.S. Congress passed ObamaCare and it was signed into law by President Barack Obama on March 23, 2010, regulations didn’t take effect until 2014. President Obama signed several executive orders hoping to save vulnerable Red State Democrats from defeat in the 2014 midterm elections.
He was unsuccessful.
Despite months of grabbling with website cronyism and incompetency, the regulations mandated by the Patient Protection and Affordable Care Act (PPACA) took effect in 2014. According to data (below) from Health and Human Services (HHS), average individual market premiums more than doubled from $2,784 per year in 2013 to $5,712 on HealthCare.gov in 2017, an increase of $2,928 or 105%.
The report found HealthCare.gov states between 2017 and 2018 saw their average premium for the second-lowest cost silver plan increase by 37%. Between 2016 and 2017, the hike in average premiums was 25%.
Administrator Verma said CMS took actions to address market stability and, as a result, competition led to more issuers, which led to lower average premiums.
In 2019, there will be 23 more medical QHP issuers than were participating during open enrollment in 2018. Further, 29 current medical QHP issuers are expanding their service area into more counties. The number of counties with only one insurer has dropped from 56% in 2018 to 39% in 2019.
Only 4 states will have only one insurer, compared to 10 in 2018.
“The president who was supposedly trying to sabotage the Affordable Care Act has proven better at managing it than the president who wrote the law,” HHS Secretary Alex Azar said recently during a speech to a health policy group in Nashville.
The state of Tennessee saw the largest drop in premiums, with the cost of that silver plan falling 26.2%. The Volunteer State is currently at the center of the battle for control of the U.S. Senate in November. Rep. Marsha Blackburn, R-Tenn., was thought to be in a tight race against former Democratic Governor Phil Bredeson.
However, the race has moved away from the Democrats in the last few weeks, as have many others on the GOP-friendly map. Healthcare continues to ascend as a top voting issue as optimism about the state of the economy increases. The PPD Election Projection Model now projects the U.S. Senate election in Tennessee Likely Republican.
About the CMS Study
To determine the year-over-year changes, CMS analyzed Exchange individual plan year 2019 premium data submitted as of September 28, 2018, as part of the QHP certification process. Average premiums were then weighted, based on 2018 Exchange enrollment data. Data is subject to change due to plan withdrawals.
[su_document url=”https://www.peoplespunditdaily.com/wp-content/uploads/2018/10/Individual-Market-Premium-Changes-HHS-CMS.pdf” width=”720″ height=”860″]






Don Easley / October 11, 2018
That’s what happens when you eliminate government mandates and require insurance companies to compete on the open market for your business! It’s really quite simple!
/